Breast Reconstruction
According to the National Cancer Institute, there will be over 250,000 new cases of breast cancer diagnosed in 2018. The majority of women diagnosed with breast cancer will undergo surgery of some kind. Options may include a removal of the cancerous area itself (lumpectomy) which is usually combined with radiation treatment, removal of the entire breast (mastectomy), or removal of both breasts (bilateral mastectomy).
After a patient receives the appropriate treatment for her cancer, which is dictated by their oncologist and breast surgeon, many women elect to undergo breast reconstruction. This can be accomplished in one of two ways: implant-based reconstruction and autologous reconstruction. Implant-based reconstruction is just that, reconstruction of the breast mound with the use of a breast implant. An autologous breast reconstruction means using your body’s own tissue to recreate a breast mound.
Options for implant-based reconstruction
- Smooth round silicone breast implant
- Textured anatomical “tear drop shaped” breast implant
A breast implant may be placed at the same time as the mastectomy “direct-to-implant reconstruction”, but more commonly in implant-based breast reconstruction a two-stage method is required by first placing a tissue expander, then after expansion of the skin (and possibly muscle) over the course of months, a permanent implant is used to replace the tissue expander during an out-patient second procedure.
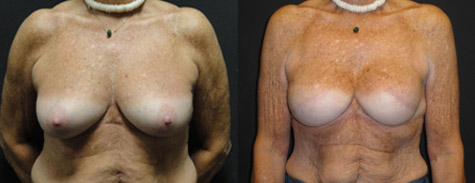
Patient pictured is 1 year postop from direct-to-implant reconstruction with 500cc silicone implants.
Options for autologous breast reconstruction
- Tissue from the back, lower abdomen, inner thigh, or buttock can be used
- Your plastic surgeon will discuss these options with you to customize your plan
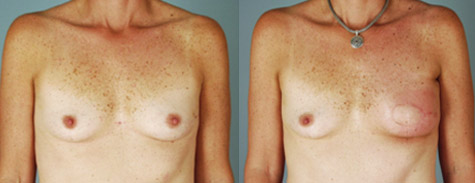
Patient pictured is 6 months postop from left breast reconstruction with a DIEP flap.
Pros of implant-based reconstruction:
- Shorter operation and hospital stay
- Less downtime and sooner return to regular daily activities
- No donor site scar
Cons of implant-based reconstruction:
- Usually require two stages
- Require routine monitoring of the implant with imaging
- Manufacturer recommends that the implant be exchanged every 10 years
Pros of autologous reconstruction:
- No prosthetic implant, so no need for routine imaging to monitor the implant
- Can give a more natural look and feel
- Usually completed in one procedure
Cons of autologous reconstruction:
- Requires donor site/scar
- Risk of donor site complication or problem with the transferred tissue
- Longer surgery, hospital stay, and recovery
The decision to undergo breast reconstruction along with the options for breast reconstruction can be an overwhelming topic at a time that is frequently the darkest period of the woman’s life. This is a discussion that should take place in a comfortable setting with a compassionate reconstructive surgeon whose goal is to create a treatment plan unique to the patient’s wishes.

